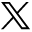Unlike most health departments, the Boston Public Health Commission oversees and operates the city’s Emergency Medical Services. The unique configuration meant that on April 15, when two homemade bombs exploded near the finish line of the Boston Marathon, public health was on the scene and ready to respond.
Hours earlier, the commission activated its Office of Public Health Preparedness and Medical Reserve Corps in accordance with its regular responsibilities at the marathon, which this year attracted about 27,000 registrants. The day of the bombings, nearly 200 Boston health department personnel were already on site, overseeing medical activities and treating runners with injuries and health problems inside medical tents set up along the marathon route. Even before the bombings, which killed three people and injured more than 260, health personnel coordinated transportation for about 70 marathon-related illnesses and injuries, said APHA member Barbara Ferrer, PhD, MPH, MEd, Boston’s health commissioner and executive director of the Boston Public Health Commission.

First responders help the wounded following explosions at the Boston Marathon in April. Boston health department personnel were already on site before the bombings to help with the marathon, which helped speed emergency medical response.
Photo by Kelvin Ma, courtesy Bloomberg/Getty Images
“We were fully staffed and ready to respond because we anticipated having more than the typical number of emergency room admissions that day,” Ferrer told The Nation’s Health. “That’s why there weren’t more lives lost.”
In the immediate aftermath of the bombings, medical and health department personnel began treating more than 140 people and coordinated hospital transportation for 90 people within 30 minutes, she said. In the hours that followed, the health department’s Stephen M. Lawler Medical Intelligence Center, a state-of-the-art communications hub, began coordinating with area hospitals to determine where patients were located and connecting them with their family and friends. It was a difficult task, as many patients were unconscious or were rushed into operating rooms, said Ferrer, who noted that it took more than 12 hours to generate complete patient lists. By 7:30 p.m. on the night of the bombings, the health department and fellow agencies had set up a drop-in center to offer counseling and support as well as to assist the thousands of runners who had traveled in from out of town and were stranded without identification or money.
“To be honest, it was too much to believe,” Ferrer said. “It was like a battlefield.”
In the days that followed, the health department continued to offer mental health counseling and support, deploying counselors to schools and community groups, to meetings with fellow first responders and to large gatherings, such as vigils. The health department also helped sift through the hundreds of offers of assistance, from people offering prosthetic limbs to those offering to build access ramps in people’s homes. Health workers even took a group of patients and families to the street where the bombings took place so they could have a moment to themselves before the street re-opened.
“It was very healing for them, but I wouldn’t have thought that’s something I would have been doing,” Ferrer said. “It’s been a real learning lesson.”
Ferrer said the health department’s preparedness plans were well executed, though there are areas in need of improvement. For example, she said it was difficult to get good patient data in the bombing aftermath, with confusion over what type of medical information is protected under privacy laws. But overall, she praised the city’s coordinated response and the hospitals that were ready to receive a surge of patients with only 10 minutes notice.
“In responding to this event, public health could not stand alone,” she said. “All these partnerships make sure your response is robust not just in the immediate aftermath, but in the long phase of recovery.”
At Massachusetts General Hospital, which received 31 people injured in the bombings, the 49-bed emergency room already had 91 patients when staff first heard of the bombings, said Paul Biddinger, MD, chief of the hospital’s Division of Emergency Preparedness. But thanks to planning and practice, staff were able to create extra capacity in mere minutes — “otherwise, it would have been impossible to take in critically injured patients in the span of 10 minutes and successfully get them to the (operating rooms)…it’s a tremendous mobilization of resources,” he told The Nation’s Health. Hospital staff kept in contact with state and local public health officials through the state’s Health and Homeland Alert Network, a secure Web portal that sends out real-time alerts.
“We’ve confirmed many things we suspected…and one is that (preparedness) exercising is absolutely key,” said Biddinger, who also serves as associate director of the Harvard School of Public Health Center for Public Health Preparedness. “Local public health and hospitals really do depend on federal funds to support planning activities and exercises and if that funding goes down, we may lose a lot of these gains.”
At the Massachusetts Department of Public Health, the Boston Marathon is typically thought of as a mass casualty exercise, said Mary Clark, MPH, JD, director of the department’s Emergency Preparedness Bureau. The day of the bombings, two bureau staff were working at the State Emergency Operations Center and more than a dozen state health workers were stationed in medical tents along the marathon route. Within a minute after the bombs detonated, a worker in the medical tent at the finish line alerted staff at the emergency operations center, which allowed the state health department to send out an alert via the Health and Homeland Alert Network just minutes later, Clark said.
Though much of the response is via local public health, the state health department acts as an information conduit and offers support as needed, Clark said. For example, state health workers coordinated additional blood supplies from Rhode Island and helped hospitals locate extra surgical and amputation kits. And because so many marathon participants did not live in Massachusetts, state health workers disseminated information to fellow state health departments about identifying mental health services for their residents.

Rescuers rush a person injured in the first of two bombings on April 15 across the finish line of the Boston Marathon.
Photo by John Tlumacki, courtesy The Boston Globe/Getty Images
“This event underscores that no single discipline can respond to an event like this,” Clark said. “A successful response requires (that) public health work closely with public safety and the health care system and having those people at the table is the only way to plan.”
Back in Boston, Ferrer noted that without the support of federal public health and hospital preparedness funds, the aftermath of the bombings would have likely been even more serious. Despite the importance of such funds, levels have been declining and President Barack Obama’s fiscal year 2014 budget proposal would cut health preparedness and response funds by another $48 million.
“I would hope that what happened in Boston serves as a good example to those who (are) making funding decisions that without past funding, this disaster could have been so much worse,” she said. “People’s lives were saved and, in part, that was because the city was so well prepared and investments were made across the board.”
To help those injured in the bombings, visit www.onefundboston.org.
- Copyright The Nation’s Health, American Public Health Association