Like other startling health statistics, the U.S. infant mortality rate easily elicits both sighs of frustration and words of determination from health workers — frustration from knowing many such deaths are preventable and determination from knowing that a poor infant mortality rate does not bode well for the nation’s future health prospects.
In response, health workers at national, state and local levels are coming together to address the issue. In Virginia, for example, health workers are harnessing their frustration and determination to bring the old proverb “it takes a village to raise a child” to life. Gathering a diverse group of stakeholders to the public health table, workers are determined to tackle “this unseen epidemic,” said Phil Giaramita, spokesman for the Virginia Department of Health’s new Commissioner’s Working Group on Infant Mortality. Faced with a state infant mortality rate that claims the lives of seven times more children each year than car accidents do, the Virginia group is busy developing community-based strategies to improve the health of pregnant women, new moms and babies. And the state isn’t alone in confronting what Virginia Gov. Tim Kaine has called the state’s “most glaring health failure.” Declines in infant mortality rates nationwide have stalled and the country’s global infant mortality ranking has, sadly, increased.
Released in October 2008, a new data brief from the Centers for Disease Control and Prevention’s National Center for Health Statistics ranks the United States 29th globally in infant mortality in 2004, the latest year such data were available for all countries. The U.S. ranking, which has risen from 12th in 1960 to 23rd in 1990, currently ties the United States with Poland and Slovakia. Authors of the brief, “Recent Trends in Infant Mortality in the United States,” noted that while such global comparisons can be affected by reporting differences, “it appears unlikely that differences in reporting are the primary explanation for the United States’ relatively low international ranking.” According to the brief, the U.S. infant mortality rate in 2005 was 6.86 infant deaths per 1,000 live births, not much different than the 6.89 rate in 2000 — a lack of decline that has “generated concern among researchers and policy-makers.” In fact, the level rate from 2000–2005 represents the first period of ongoing lack of decline in the U.S. infant mortality rate since the 1950s, the brief stated. The Healthy People 2010 target for infant mortality is 4.5 infant deaths per 1,000 live births.
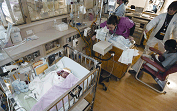
Premature infants receive care at a New York City medical center in 2004. Increasing premature births is one of the reasons for the high infant mortality rate in the United States.
Photo by Mario Tama, courtesy Getty Images
In 2005, 28,000 infants younger than age 1 died, out of more than 4.1 million births. Among those deaths were glaring disparities: The brief reported that the infant mortality rate was 13.68 deaths per 1,000 live births among blacks in 2005, 8.06 among American Indians and Alaska Natives, 8.3 among Puerto Ricans and 5.76 among whites. The lowest U.S. rate was among Cuban Americans, at 4.42. While a number of factors can contribute to such disparities, such as access to care and socioeconomic status, the brief’s authors found that “many of the racial and ethnic differences in infant mortality remain unexplained.” However, one factor researchers know is affecting U.S. infant mortality rates is preterm birth. In 2005, more than 68 percent of infant deaths occurred among preterm infants, up from more than 65 percent in 2000. In November, the March of Dimes released its first annual “Premature Birth Report Card,” giving the nation an overall “D” grade and noting that preterm birth — birth before 37 weeks of gestation — is the top cause of death in an infant’s first month of life.
“Our lack of progress really is related to more and more babies being born too small,” said Joann Petrini, PhD, MPH, director of the March of Dimes’ Perinatal Data Center. “Because of amazing high-tech care, thankfully, we see miraculous outcomes for very, very small babies…but it can make it difficult to communicate that prematurity is still a problem.”
Forty weeks is the normal length for pregnancy, but even babies born between 34 weeks and 36 weeks — known as late preterm — have a death rate three times that of full-term babies, said Petrini, adding that “40 weeks is 40 weeks for a reason.” Petrini said an increase in late preterm births has been driving up the overall preterm birth rate, which NCHS reported in January rose to 12.8 percent in 2006, up 36 percent since the early 1980s. Babies born premature can later suffer a number of problems, including developmental disabilities, hearing loss, blindness and chronic diseases such as asthma. Though many behavioral factors, such as smoking, lack of breastfeeding and a rise in medically unnecessary Caesarean sections, are known to contribute to the U.S. infant mortality and prematurity rates, much is unknown.
“We need more research to understand the causes of prematurity… there’s still a lot we don’t know,” Petrini told The Nation’s Health. “You can do everything right and still have a preterm baby.”
Petrini, an APHA member, described the prematurity and infant mortality rates as representing a microcosm for a number of public health issues: helping women access needed health services, supporting smoking cessation, ensuring pregnancies are planned and educating nontraditional public health partners that they too can support maternal and child health. After all, healthy mothers make for healthy babies, said Judy Meehan, executive director of the National Healthy Mothers, Healthy Babies Coalition, a leading maternal and child health resource and advocate with more than 20 state and local coalitions throughout the country.
“It’s so complex because there’s two patients,” Meehan said. “In every respect, if the mother is doing well, the baby will do better.”
Meehan also said “more research (is needed) to examine this problem of babies being born too small and too soon before we’ll see change.” Moreover, education and partnerships are key, she said.
“Our challenge is to get the information into the hands of those who need it most, to make sure that we’re educating in order to make real behavior change,” Meehan told The Nation’s Health. “Our coalition and a lot of those in the public health arena recognize that there has to be communication across the disciplines…We have to work at public- private partnerships to make this happen and it’s going to take real mobilization on the part of (maternal and child health) advocates.”
Public health ready to make a difference
In Nashville, Tenn., Kimberlee Wyche-Etheridge, MD, MPH, can see first-hand the long road toward healthier mothers and babies for all communities. Director of the Bureau of Family, Youth and Infant Health at the Metro Nashville Davidson County Public Health Department, Wyche-Etheridge said she is “saddened but not surprised” at the U.S. infant mortality ranking. Tennessee’s infant mortality in 2006 exceeded the national rate by more than 31 percent, according to the state health department, with the black infant death rate more than twice that of white infants. The March of Dimes reports that Tennessee’s preterm birth rate increased 13 percent from 1995 to 2005.

Photo by Andrea Gingerich, courtesy iStockphoto
“We continue to focus and put more resources into intervention and not into prevention,” said Wyche-Etheridge, who co-chairs the APHA Maternal and Child Health Section’s SIDS/Infant Mortality Committee. “So we have wonderfully funded, top-notch (neonatal care units), but preconception health isn’t covered by insurance in most cases. We put out resources after the fact.”
Like her fellow advocates, Wyche-Etheridge called for heightened attention to making sure women are healthy before pregnancy. More time should be spent reaching young women with healthy behavioral messages, not just in the medical office, but in schools and churches, she said, adding that “these messages would be more mainstream, but we tend to continue to shun anything having to do with reproductive health and our young ladies and men grow up without the basic knowledge to be healthy adults.” Additional state and federal funding would also help, Wyche-Etheridge said, as fewer and fewer health workers try to reach more people.

The high U.S. rate of infant mortality is not decreasing as much as advocates hope, with 6.86 deaths for every 1,000 live births.
Photo by Don Bayley, courtesy iStockphoto
“Health is a lifetime issue and if we can stop focusing on the periodic issues then we may actually see some change in infant mortality,” she told The Nation’s Health. “We spend a lot more on keeping people out of the grave than in the cradle.”
Back in Virginia, the state’s infant mortality working group — which includes stakeholders ranging from health care providers to civic organizations to retailers — hopes to release a game plan to raise public awareness early this year, Giaramita said. Much of the group’s educational messaging will focus on the healthy behaviors known to reduce the risks of poor infant health, such as smoking cessation and obesity prevention, Giaramita said, noting that the “same issues Americans have in trying to live healthy lifestyles are magnified when talking about pregnant women.”
And such education has a proven track record: The Virginia Department of Health’s Resource Mothers Program, which has been matching lay community health workers with pregnant teens for the past few years, has been effective in decreasing infant deaths and disabilities and enhancing the health of pregnant teens. Unfortunately, while the program has seen success in helping low-income teens with issues such as accessing prenatal care and realizing the importance of breastfeeding, there is simply not enough funding to help all those who need it. Hopefully, though, the state working group’s plan can mobilize communities to start filling in the gaps.
“Traditionally, it’s said that you can measure how seriously your community cares about health by looking at the infant mortality rate, and it’s easy to make that conclusion because the factors that contribute to infant mortality have health implications for everybody,” Giaramita said. “The kinds of healthy behaviors that lead to healthy babies lead to healthy citizens.”
For more information on U.S. infant mortality, visit www.cdc.gov/omhd/AMH/factsheets/infant.htm or www.marchofdimes.com.
- Copyright The Nation’s Health, American Public Health Association