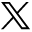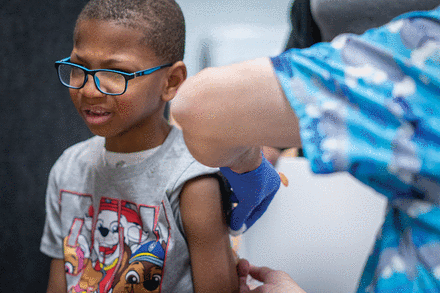
Xerius Jackson receives an MMR vaccine at a Lubbock Public Health Department clinic in March in Texas. Federal funding cuts have led to cancellation of many pop-up state clinics.
Photo by Jan Sonnenmair, courtesy Getty Images
“These cuts can have a huge impact in rural areas and at small health departments. One staff person is critical, doing multiple jobs.”
— Phil Huang
This spring, the Trump administration abruptly revoked millions of dollars earmarked for state and local preparedness by the U.S. Department of Health and Human Services. While the decision was made at the federal level, its fallout was quickly felt in communities across the U.S.
“This unprecedented work has stopped public health in its tracks,” Lori Freeman, MBA, CEO of the National Association of County and City Health Officials, said during a March briefing. “All this is done without any consultation with public health partners or Congress.”
On March 24, HHS, under the leadership of Secretary Robert F. Kennedy Jr., canceled nearly $12 billion in public health funding for local and state agencies. Congress had allocated the funds for pandemic preparedness, mental health, overdose prevention, community health programs and infrastructure upgrades.
In the wake of the decision, programs focused on gun violence, opioid use, climate health, maternal health, prevention of injuries and more were eliminated or devastated at local departments of health across the U.S.
California lost five federal grants worth over $700 million. The rescinded funding supported gaps in its public health infrastructure, including ongoing responses to COVID-19 disease and other respiratory and vaccine-preventable diseases, Erica Pan, MD, California Department of Public Health director and state public health officer, said in a news release.
For New York, the cancellation would cost the state over $400 million in funding.
“Slashing this funding now will reverse our progress on the opioid crisis, throw our mental health systems into chaos and leave hospitals struggling to care for patients,” Lititia James, the state’s attorney general, said in a news release.
Some health departments lost their mobile health units and were unable to complete surveillance research on infectious diseases, Freeman said.
Public Health-Seattle and King County was notified of revocation of several grants, one of which funds the salaries for 45 community health workers assigned to vulnerable communities in the Washington county.
“We spent years training them and embedding them in communities across the region,” Faisal Khan, MD, the agency’s director of public health, said during a media briefing.
Even if funding is restored in six months or one year, the program will have to start from scratch, not where it left off, he said. The health workers will have moved on.
In Texas, the Dallas County Health and Human Services department was notified that three federal grants would stop. Vaccination, epidemiology, technology modification and staffing were impacted, even as the state wrestled with a major measles outbreak, Phil Huang, MD, MPH, director and health authority of the Dallas health agency, said at a briefing.
Eleven full-time workers and 10 part-time workers involved in infectious disease surveillance and delivering routine child vaccinations were laid off, he said. Over 50 immunization clinics at schools and in communities had been canceled in Dallas County.
Smaller health agencies were experiencing even greater loss because of the funding rescission, even if it was only one or two workers being let go.
“These cuts can have a huge impact in rural areas and at small health departments,” Huang said. “One staff person is critical, doing multiple jobs.”
Though a federal judge on April 4 temporarily barred HHS from rescinding federal funding promised to local and state public health agencies, the damage was already done.
For more information, visit www.naccho.org.
- Copyright The Nation’s Health, American Public Health Association